The Humbling Gift
What an Achilles rupture taught me about the other side of the weight room
I didn’t hear a pop. Didn’t hit the ground.
It felt like someone had kicked me in the back of the lower leg. Hard. I turned around to see who it was.
Nobody was there.
That’s when I knew something had gone wrong.
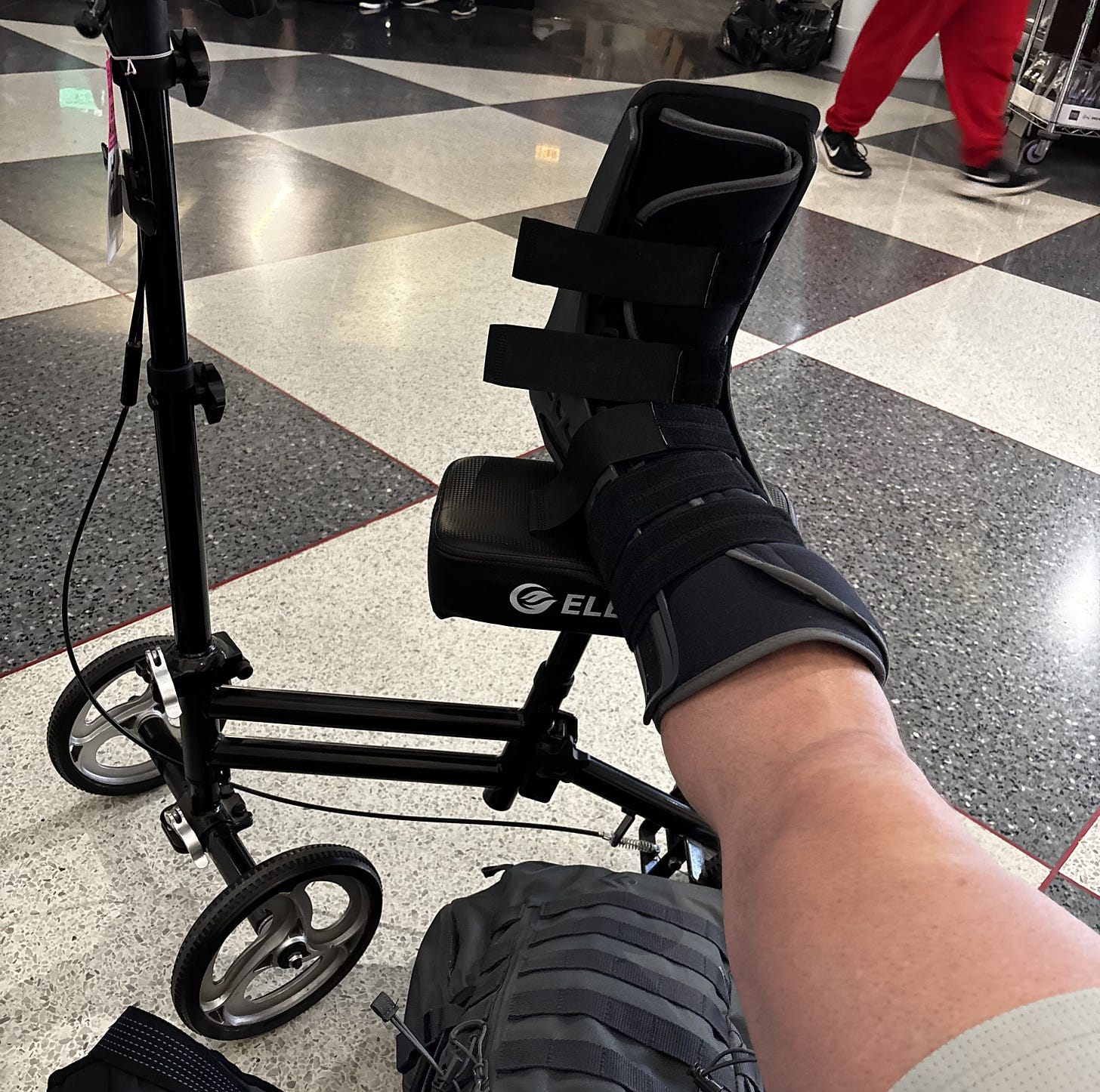
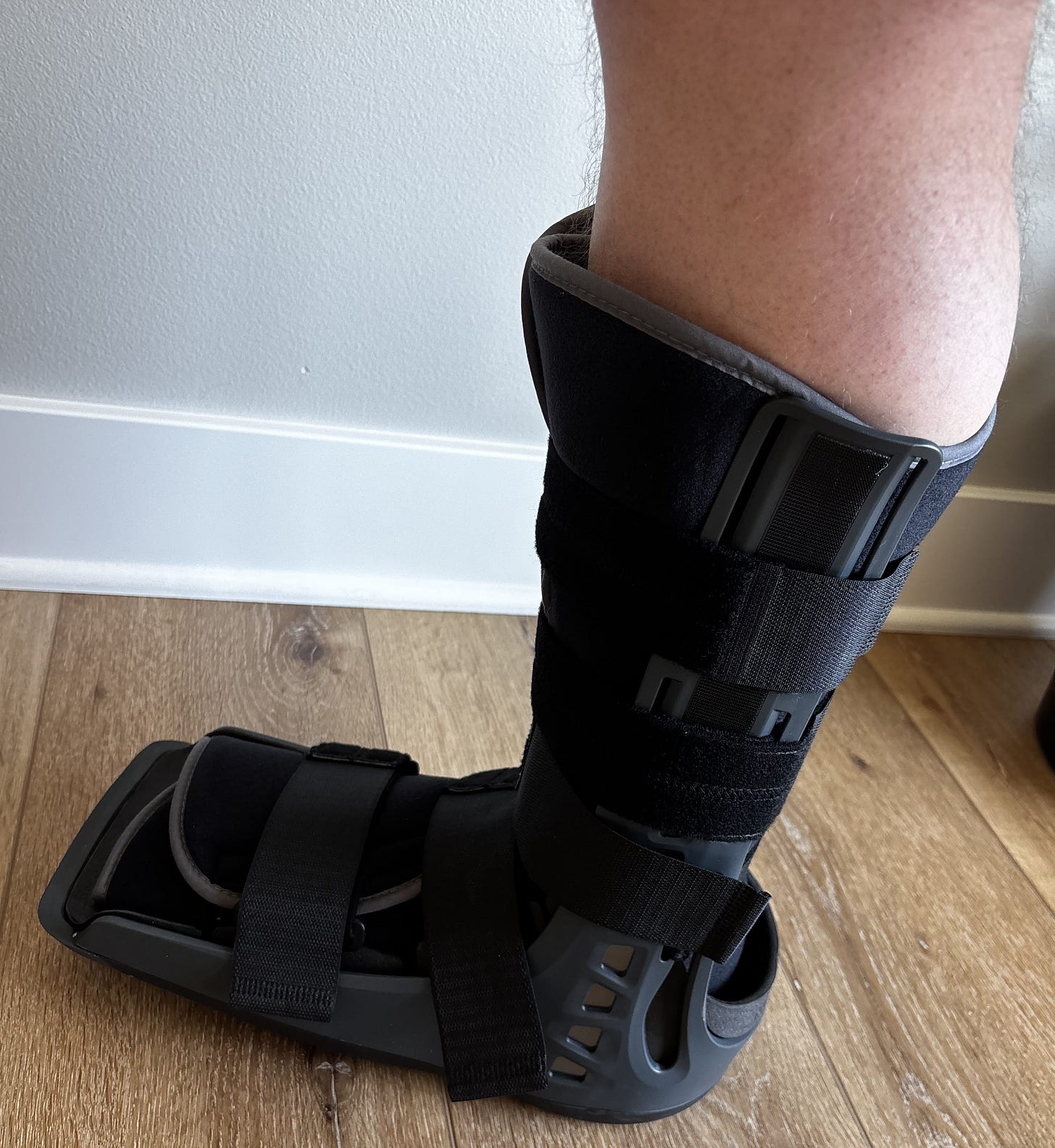
Nearly a year ago, I tore my Achilles tendon. Surgery followed. Then a boot. Then months of relearning what my body could do. Things that once required no thought, standing up from a chair, walking to the mailbox, loading a bar, suddenly required planning.
That’s a strange thing to sit with when you’ve spent your career telling athletes how to move.
The Achilles is the largest, strongest tendon in the human body. It handles enormous loads, particularly during the explosive, high-velocity movements that define athletic performance. When it ruptures, the consequences are serious. Research on professional athletes shows that nearly one in four can’t return to their sport at all, and those who do typically need close to 11 months of rehabilitation, nearly double what’s estimated for the general population. Performance metrics decline. Career length shortens. The injury leaves a mark.
I’m not a professional athlete. But that data lands differently when you’re living the recovery.
The Reckoning
I want to be honest about the early weeks. I didn’t spiral into depression, but I wasn’t okay either. I was frustrated in a way that felt disproportionate, frustrated at the pace, at the limitations, at the body that had carried me through decades of hard training and was now asking me to slow down.
I’ve talked to enough athletes to know that frustration is almost always the first layer. Under it, if you’re willing to look, is something quieter. Fear. Not fear of the injury itself, but fear of what it might mean.
I’m in my mid-forties. That fact sat with me in a way it hadn’t before. I’ve always been active. Always trained. Always identified, at least in part, as someone who could do physical things at a high level. The injury didn’t just sideline me. It forced a conversation I’d been quietly avoiding.
You can know intellectually that you’re aging. You can see it in the mirror, feel it in recovery time, notice it in the way your joints talk to you the morning. But there’s a difference between knowing it and being confronted with it. A major surgery in your mid-forties has a way of making it concrete. The body isn’t just asking you to slow down for a few weeks. It’s telling you something about the arc you’re on.
That’s not despair. But it sits with you.
There’s grief in it, if you’re honest. Grief for the version of yourself that didn’t have to think about this yet. Grief for the assumption that the physical capacity you’d built would just be there, reliably, indefinitely. Nobody tells you that part. The rehab literature covers fear of reinjury and motivation and return-to-sport timelines. It doesn’t spend much time on the quieter reckoning that happens when a middle-aged person realizes that some of what they’ve lost may not fully come back.
That’s the thing about being on the other side of the weight room. The athletes you coach are mostly young. Their bodies are forgiving. Their timelines are different. When you tell a 17-year-old to trust the process, you mean something different than when you’re telling yourself the same thing at 44 with a repaired tendon and an arthritic shoulder.
The humility wasn’t just about the injury. It was about the stage of life it landed in.
There’s a name for the psychological side of that fear. Researchers call it kinesiophobia, an excessive, irrational fear of movement due to concern about reinjury. It sounds clinical. Lived, it’s just the reluctance to fully trust the leg again. Studies on Achilles tendon recovery have found that patients who report higher fear of reinjury show significantly lower functional outcomes, lower activity scores, lower quality of life, and poorer physical performance measures. In one large cohort of 550 patients, those who reported fear of reinjury scored 15 points lower on the standard Achilles rupture outcome scale than those who didn’t.
The mind isn’t separate from the rehab. It is the rehab.
The Other Side of the Table
I’m just past the midpoint of my coaching career. I’ve got shoulder arthritis. Now a surgically repaired Achilles. The math isn’t complicated. The body is keeping score in ways I didn’t think much about when I was younger.
That reckoning, uncomfortable as it was, turned out to be useful.
My physical therapist was a recent grad. Young. Confident without being arrogant. Good at his job in that specific way that new practitioners sometimes are, not yet worn down, still curious, still asking why.
He figured me out quickly.
He knew I was competitive. He knew I had a coaching background. So he used it. At one point, he mentioned that a younger client had hit a specific benchmark in recovery and cited the number. He didn’t push. He just let it land.
It landed. I trained harder the next session.
What he did wasn’t accidental. Research on Achilles recovery has found that psychological readiness to return to sport at 6 and 12 months post-injury is significantly associated with actual sports participation and performance outcomes. Motivation levels, confidence, and reduced fear of movement aren’t soft variables. They’re predictive ones. A skilled PT doesn’t just manage tissue. He manages the mental environment around the tissue. My therapist was doing both, whether he framed it that way or not.
Looking back, that’s exactly what a skilled coach does. He read what motivated me, then deployed specific, targeted information to trigger something he already knew was there. I’ve tried to do that same thing with athletes hundreds of times. Experiencing it from the other side was something else entirely.
There’s a concept the cook-to-chef framework keeps coming back to: understanding not just what works, but why it works. You can run a program that produces results without being able to explain the mechanism. Real mastery requires both.
The injury applied that same test to me as an athlete, not a coach.
I knew what rehabilitation was supposed to look like. I had the framework. What I didn’t have was the experience of being inside it, of actually needing someone else to pace the process, to set the standards, to say “not yet” when I was ready to push.
Being coached well is its own kind of education. Research on the coach-athlete relationship consistently shows that empathy and perspective-taking are core competencies. Coaches who can see the world through their athletes’ eyes make better decisions, build more trust, and create more productive training environments. The gap between knowing that intellectually and having lived through a year of relearning how to walk is significant.
I think I’m a better coach for having been a patient.
For strength coaches specifically, this has a concrete application.
A qualitative study on Achilles rupture recovery identified the central theme of what patients needed as: “Help me and then I can fix this.” Athletes described the critical importance of social support from their care team, an environment that fosters trust, and clear, honest communication about what to expect. Mental acceptance of the injury, preparing for the long road rather than resisting it, consistently accelerated recovery. Previous injury experience helped. Framing the timeline realistically helped. Feeling supported helped.
That’s not a medical insight. That’s a coaching one.
When you have an athlete in your weight room who’s rehabbing a significant injury, the physical protocol matters. But the research is clear that psychological readiness, motivation, and fear of movement are independent predictors of outcome. Those variables are shaped by the environment you create and the relationship you build. A coach who’s been on that side of the table, even once, understands that in a way that no certification covers.
I wouldn’t wish injury on anyone.
But I’ve stopped viewing this one as purely a setback. Something came out of it. A closer relationship with patience. A more genuine empathy for athletes in recovery. A reminder that the body has a timeline that isn’t negotiable, regardless of what your training history looks like or what your ego wants.
The athletes navigating serious injury in your program aren’t just rehabbing tissue. They’re reconfiguring their relationship with what their body can and cannot do, sometimes permanently. That deserves more than the speech about trusting the process. It deserves someone who has been humbled enough to really mean it.
I’m almost a year out. The Achilles is holding. The shoulder still complains on heavy pressing days. I’ve made adjustments.
The coaches who can’t adapt are the ones who built their identity too tightly around a single version of themselves.
The body eventually asks everyone to let go of something. The question is whether you grip tighter or get curious about what’s next.
I’m trying to get curious.
Until next time,
References
Jónsdóttir, U. S., Brorsson, A., Nilsson Helander, K., Tranberg, R., & Larsson, M. E. H. (2023). Factors that affect return to sports after an Achilles tendon rupture: A qualitative content analysis. Orthopaedic Journal of Sports Medicine.
Larsson, E., LeGreves, A., Brorsson, A., Eliasson, P., Johansson, C., Carmont, M. R., & Nilsson Helander, K. (2024). Fear of reinjury after acute Achilles tendon rupture is related to poorer recovery and lower physical activity postinjury. Journal of Experimental Orthopaedics.
Lorimer, R., & Jowett, S. (2013). The development of empathic accuracy in sports coaches. In Jones et al. (Eds.), The Sociology of Sports Coaching. Routledge.
Morales-Asencio, J. M., et al. (2021). Psychological factors change during the rehabilitation of an Achilles tendon rupture: A multicenter prospective cohort study. Physical Therapy.
Vivekanantha, P., et al. (2023). Kinesiophobia contributes to worse functional and patient-reported outcome measures in Achilles tendinopathy: A systematic review. Knee Surgery, Sports Traumatology, Arthroscopy.
Williams, G., et al. (2021). Career outlook and performance of professional athletes after Achilles tendon rupture: A systematic review. Foot & Ankle International.